New research published in the New England Journal of Medicine shows that the respiratory virus SARS-CoV-2, which causes COVID-19, is also responsible for severe damage to blood vessels increasing the risk of blood clots. One Amsterdam study found that almost one-third of patients hospitalized with severe COVID-19 demonstrated complications from blood clots.
A blood clot is a clump of blood formed when blood changes from a liquid to a thicker gel-like state. Ordinarily, this can be a life-saving mechanism to help stop bleeding; however, when the clot breaks off, it can travel through the bloodstream choking the supply of blood to essential organs such as the lungs (causing a Pulmonary Embolism) or the brain (causing a stroke).
Patients admitted to the hospital are more likely to have blood clots in the blood vessels of the legs due to immobility while hospitalized. Staying active, use of compression stockings, sequential compression devices, and, in select cases, the use of blood thinner can help lower the risk of clots.
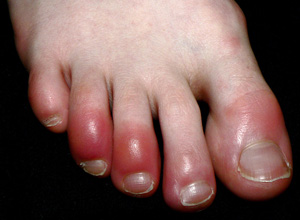 There are also reports of blood clots in patients with COVID-19 who are at home and staying active. Swelling in the legs is the most common sign of blood clots. Some patients with COVID-19 develop a condition called “Covid toes” – red, swollen toes that may be due to small clots in the blood vessels of the feet.
There are also reports of blood clots in patients with COVID-19 who are at home and staying active. Swelling in the legs is the most common sign of blood clots. Some patients with COVID-19 develop a condition called “Covid toes” – red, swollen toes that may be due to small clots in the blood vessels of the feet.
If you have leg swelling, pain in the legs, or any other sign of a blood clot, please call us at 816-396-0245 to have a duplex ultrasound screening test for blood clots. This is performed in the comfort of the office setting at Alsara Vein Clinic.
Leg Ulcers (Sores)
Venous Ulcers
Chronic venous insufficiency (CVI) affects millions of people. In more advanced stages, it can lead to skin damage and open sores called venous ulcers—a serious but treatable condition.
We are grateful to our patients for consenting to the use of these images for educational purposes. Every effort has been made to remove all identifying information in accordance with privacy and confidentiality standards.
Why Leg Wounds Don’t Heal
Venous ulcers are not just “skin problems”—they are caused by underlying vein disease.
When pressure builds up in the veins:
- Fluid leaks into surrounding tissue
- Skin becomes inflamed, fragile, and easily damaged
- Oxygen and nutrients cannot reach the area effectively
- The body struggles to repair the wound
- Persistent itching can lead to scratching and skin breakdown
- Bacteria on the skin can enter, causing repeated infections (cellulitis)
Even with proper wound care, healing is often slow or incomplete if the underlying vein problem is not treated.
Why Treating the Veins Matters
Compression (stockings or wraps) helps improve blood flow and reduce swelling. It is an important first step—but it does not fix the root cause.
Research shows:
- Treating abnormal veins helps wounds heal faster
- It significantly reduces the risk of recurrence
- Without vein treatment, ulcers often return—in up to 45–70% of cases
In other words, the wound may close temporarily, but the underlying problem remains—leading to repeated breakdown.
Why Early Evaluation Matters
Vein disease is progressive, meaning it can worsen over time if left untreated. What may begin as mild symptoms can progress to skin damage or ulcers.
In severe cases:
- Infection can spread into the bloodstream (sepsis, life-threatening)
- Infection can involve the bone (osteomyelitis, limb-threatening)
A simple, painless ultrasound can:
- Identify the underlying cause
- Map the affected veins
- Help create a personalized treatment plan
The Good News: Modern Treatments Work
Modern vein treatments are:
- Minimally invasive
- Performed in the office
- Quick, with little downtime
Common options include:
- Endovenous laser ablation (EVLA)
- Medical adhesive closure (VenaSeal)
- Ultrasound-guided sclerotherapy
Often, a combination of treatments is used to close unhealthy veins and restore normal blood flow.
For patients with ulcers or advanced disease:
- Healing improves when vein issues are treated early
- Pain, swelling, and skin damage can significantly improve
- The risk of recurrence is much lower
Call to Schedule a Consultation Today!
If you have sores on your legs that won’t heal, keep coming back, or have been blamed on conditions like diabetes, eczema, or psoriasis—and you’ve been dealing with long-term wound care—there may be an underlying vein problem.
The good news is that modern vein treatments are safe, performed in the office, require little to no downtime, and are designed to keep discomfort to a minimum.
Don’t lose hope. Treating the root cause can help your wounds heal and provide lasting relief. Call us today at 816-396-0245 to schedule a Consultation with your Venous Ulcer Specialist at Alsara Vein Clinic.
Varicose Vein Treatments are coved by insurance including Medicare and Medicaid
Vein Disease Menu

 There are also reports of blood clots in patients with COVID-19 who are at home and staying active. Swelling in the legs is the most common sign of blood clots. Some patients with COVID-19 develop a condition called “Covid toes” – red, swollen toes that may be due to small clots in the blood vessels of the feet.
There are also reports of blood clots in patients with COVID-19 who are at home and staying active. Swelling in the legs is the most common sign of blood clots. Some patients with COVID-19 develop a condition called “Covid toes” – red, swollen toes that may be due to small clots in the blood vessels of the feet.
